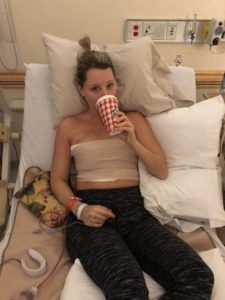
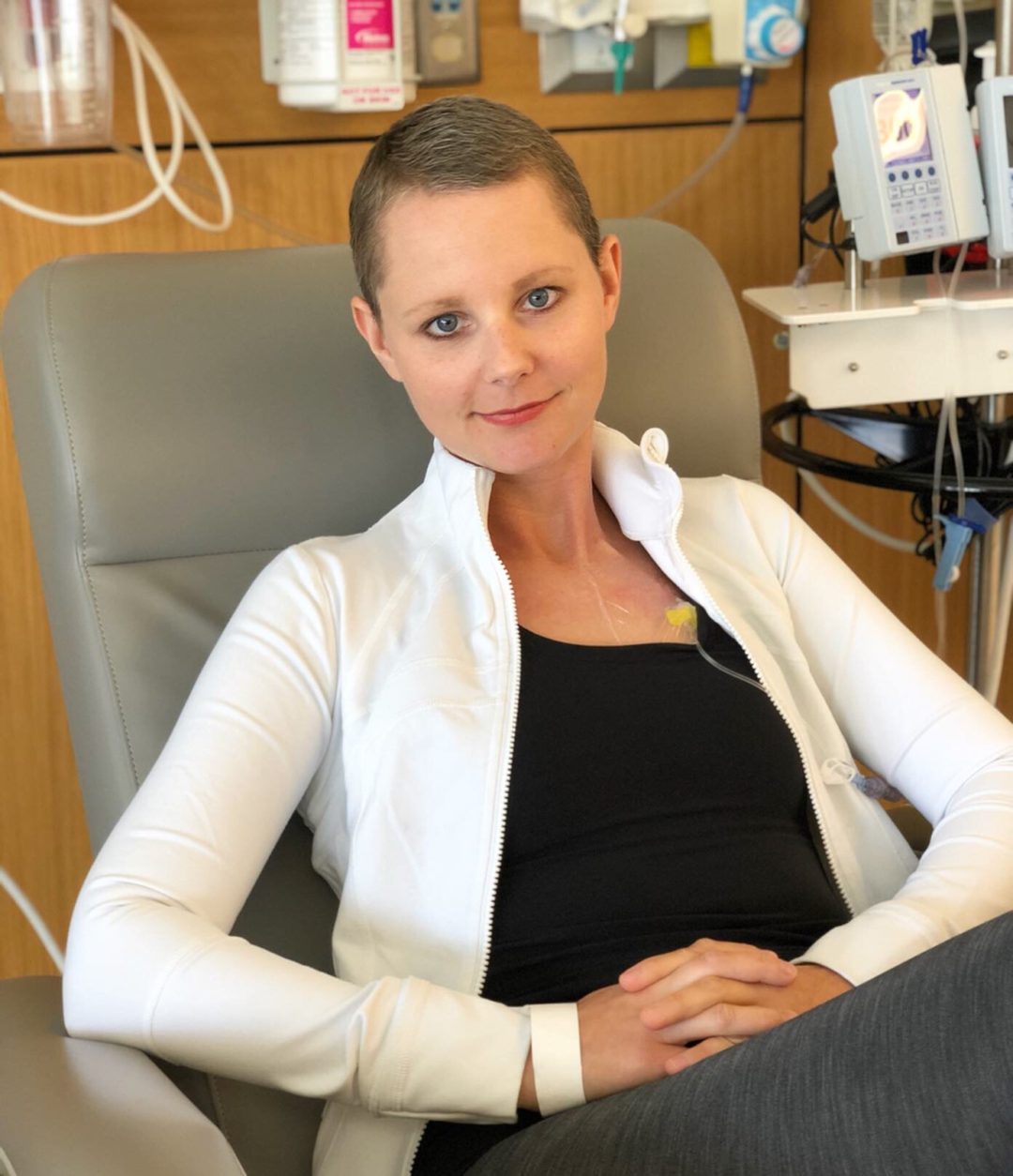
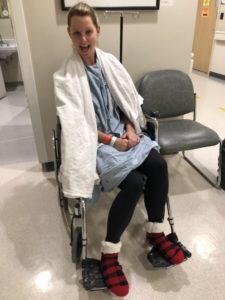
I’m hoping this is going to be one of the last health updates I have to give for a very long time, simply because I’m hoping I won’t have much to say about it moving forward. But I do have something to say about the recovery process in general.
The last couple weeks have been a bit of a roller coaster, sure. But today I stand here in a good place, with a body that isn’t hurting very much. My mood has been up and down on my way here, and my brain has been seriously overthinking every aspect of my life – but I can happily say that pain doesn’t seem to be a major issue for me right now, and that is a good thing.
The cortisone shot I got at the rheumatology office was pretty great, to say the least. I was feeling SO good – hyper – energetic – wildly optimistic about life – but then I crashed. On day 7 I woke up and I didn’t feel good, and my body hurt. The depression quickly followed, because I knew the effects of the shot had worn off, but worse I realized that everything I had been feeling was definitely because of that shot, and not because I had finally gotten back to normal.
Normal. There is that word. I’ll get to that in a minute.
I was told the shot would have an effect for 2-3 weeks, and I was disappointed that it only lasted one week for me, but at least now I knew I had another tool in my pocket. I called the office to let them know that it worked, and to book another appointment to have it again. Then the disappointment and borderline anger came when the receptionist delivered the news that these shots can only be administered a few times a year. What.
This is another example of a key piece of information being left out of the initial conversation with my doctor. Why does it seem like I keep getting half of the story when I’m making decisions about my health? I was frustrated, I’m still frustrated. I try to put myself in my doctor’s shoes – maybe most patients don’t need to know, don’t ask, don’t care… maybe they think it isn’t an important part of the conversation or maybe they straight up forgot – after all, they’re human too. But whatever it is, I feel like my emotions around it all could have been managed if I had all the information.
So, this shot is only a once in a while thing. Cool. Not great, but it’s something I’ll remember if I need it in the future for important events or really bad stretches of pain or symptoms. You risk damaging all the tissue surrounding the injection sites, and it isn’t reversible once the damage is done. Essentially you could create new pain and issues down the road just trying to treat the current pain and issues you’re experiencing now. Good to know. Kind of important. Noted. Check. Thank you.
Then over the next couple of weeks I felt my symptoms dissipating. Every day I felt a little better, and the pain became less and less. I found myself forgetting that I even had pain a lot of the time, or I’d realize ‘hey, I don’t feel pain right now, weird’. It’s like I am afraid to be excited or happy about it, because that’s usually when something happens to pull me backwards back into it all. So that’s where I’m at right now. A cautious optimism that maybe all I needed was WAY MORE time then I was ever prepared for, to recover from all the cancer treatments, surgeries and accompanying complications.
What about my implants? Well, I honestly believe they will need to come out at some point – and probably sooner than later, but not right away. Although the pain has improved drastically, I am definitely not feeling my best. When I say that, I mean I believe that I can feel better – and I believe some less-pressing-yet-persistent symptoms are likely caused by the fact that my body is having some kind of reaction to the foreign objects inside my body. These plastic things full of chemicals are likely preventing me from my best state of health. It honestly creeps me out when I think about it, but I’m not ready. I’m not there. It’s hard being that honest with myself, never mind other people – but there it is. I’ll get there, but I’m still holding on to the idea that I’ll continue to feel better and better, and maybe if I wait just a little longer I won’t have to worry about it. After all, the doctors all tell me the implants are safe.
When I think back, and when I think WAY back, I was always told that after treatment everything would be over. I’d be back to normal, good to go, I can move on, my old life would be waiting for me. So when that never happened it affected me deeply. I worried that there was something wrong with me. I worried I didn’t do it right, or that others were better at moving on then I was. I worried about pretty much everything and it dominated my thoughts. In short, it didn’t feel good to not feel good. It’s like I had to deal with the physical aspects, but worry even more about how I FELT about it all. Like there is a right way and a wrong way to recover.
There is a huge gap in care after cancer. Because it pretty much doesn’t exist as a part of our formal treatment, and there really isn’t much direction to go seek it out on our own either. If my doctors shared some messages differently at the end of our time together I believe it would have been different for me. If my surgeons changed their messaging around my recovery then I know things would have been different for me, and it would have been easier to manage my expectations around it all. Here are a few things I would have liked to have heard, now that I look back. If you’re in my shoes now, or will be soon, or might be one day, or have a loved one in the middle of it all – here they are.
From my oncologists:
Hey Lindsy, you’re going to need ongoing support for a really long time now that your treatment is over – don’t be worried, don’t feel ashamed about it, it’s normal and everyone recovers differently. In fact, some people and most people never feel back to normal, they learn to live with a new version of normal – but one thing I can promise is that it will eventually feel normal to you and you’ll be happy. And although some people can move on from treatment without many long term physical effects, there are lots of people who experience them for months or years. Here are some resources to help you if you’re one of them.
From my surgeons:
Hey Lindsy, this is an intense and life altering surgery. If there are complications, it’s even more involved. It’s going to be a longer recovery than you’ll probably expect, but it’ll be worth it. The recovery doesn’t end when the wounds heal, it is a process of getting to know your new body and learning to work with it. It will not be the same, it won’t ever be the same, but it’s what you have to work with, and you will be able to make it work. Depending on what your expectations are, the time will vary, so let’s talk about your expectations so we can properly prepare you. Here are some resources to help you.
I can go on. And maybe I will. I think these messages can help others who feel the same way I do. Physical pain and complications are inevitable and very real – but how we react to it, feel about it and let it affect our mental health is the real area of concern here. There is a difference between pain and suffering. Pain is pain, but how we suffer from it is what really affects how we live our lives, and how we let it control our thoughts.
There is an opportunity to improve how we send our cancer patients and survivors out into the world, because I have experienced the gap first hand, and I hear about it all the time from others in the cancer community too. I know our system is doing the best they can most of the time, and the care I received during treatment was amazing, and I’m here today typing this article out as proof – but we can always do better. More information and resources, better communication, and a focus on mental health is where we start.